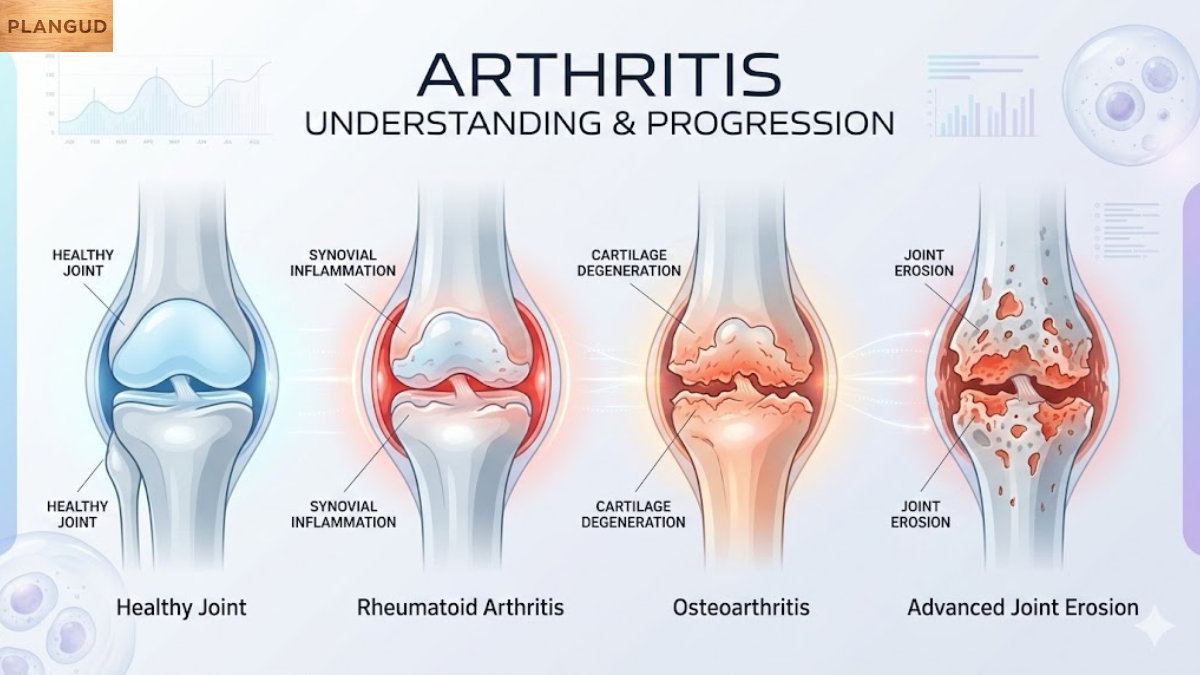
If you’re searching for what arthritis is, understanding arthritis symptoms, and exploring the most effective arthritis treatment, this guide provides medically grounded, experience-driven clarity. Arthritis is a chronic joint condition that leads to joint pain, joint stiffness, and joint inflammation, often resulting in reduced range of motion and long-term joint degeneration. It can develop gradually through cartilage wear and tear or arise from autoimmune disease, metabolic imbalance, or viral infections such as COVID-19.
Leading institutions like the Cleveland Clinic and specialized departments such as Rheumatology Care and Rheumatology Care for Children emphasize early evaluation because untreated joint damage may eventually require advanced interventions like arthroplasty or joint replacement. Understanding causes, risk factors, diagnosis, and management options empowers better long-term outcomes.
What Is Arthritis?
Arthritis refers to a group of disorders affecting the joints, where protective cartilage cushioning breaks down, or inflammation damages joint structures. Healthy joints allow smooth movement and stable joint mobility, but with arthritis, inflammation, structural degeneration, or immune dysfunction, that balance is interfered with.
Some forms are mechanical, while others result from immune system damage. Over time, this may lead to progressive joint degeneration, stiffness, and mobility limitations. Because it is a chronic joint condition, management focuses on slowing progression and protecting function rather than curing the disease outright.
Common Symptoms of Arthritis
The most recognized arthritis symptoms include persistent joint pain, morning joint stiffness, swelling, warmth near the joint, tenderness, and reduced range of motion. Many patients describe stiffness in the morning that improves with movement.
In inflammatory types, people experience recurring flare-ups or pain flare-ups, where discomfort intensifies temporarily. Some notice difficulty moving, decreased grip strength, or limitations that create a real impact on their daily routine. Over time, unmanaged inflammation may cause visible joint changes and measurable joint damage.
Types of Arthritis
There are more than 100 forms, but several dominate clinical diagnoses and align with common search intent around types of arthritis.
Osteoarthritis
Osteoarthritis is the most common form and develops due to cartilage wear and tear associated with aging or repetitive stress. The gradual breakdown of cartilage reduces shock absorption, leading to bone friction and progressive joint degeneration.
It frequently affects knees, hips, hands, and the spine. Lifestyle factors such as obesity increase mechanical stress on joints, accelerating damage.
Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune disease where the immune system mistakenly attacks joint tissue. Unlike mechanical degeneration, this form is driven by systemic inflammation. It may lead to symmetrical joint involvement and long-term joint damage if untreated.
Early use of Disease-modifying antirheumatic drugs (DMARDs) significantly improves prognosis and reduces structural deterioration.
Psoriatic Arthritis
Psoriatic arthritis occurs in individuals with psoriasis. This inflammatory form combines skin symptoms with joint involvement and may cause both pain and visible swelling.
Gout
Gout results from elevated uric acid levels, known medically as hyperuricemia. Excess uric acid forms sharp uric acid crystals inside joints, triggering sudden and severe inflammation. Diagnosis often relies on blood tests confirming high uric acid levels.
Ankylosing Spondylitis
Ankylosing spondylitis primarily affects the spine and lower back. Chronic inflammation may reduce spinal flexibility and, in severe cases, require surgical intervention such as spinal fusion.
Juvenile Arthritis
Juvenile arthritis affects children under 16. Because it occurs during developmental years, early management is essential to prevent growth-related complications.
Causes and Risk Factors of Arthritis
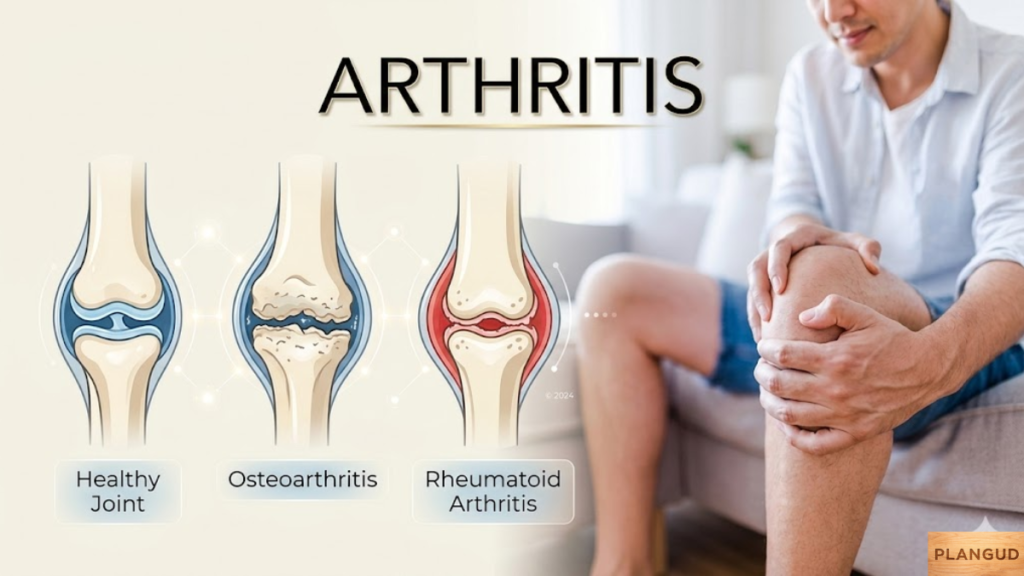
The underlying arthritis causes vary by type. Mechanical stress contributes to Osteoarthritis, while autoimmune diseases drive inflammatory forms such as Rheumatoid arthritis. Hyperuricemia causes Gout, and certain viral infections may trigger viral arthritis.
Key risk factors include age over 50, family history, obesity, tobacco use, and repetitive joint strain. Environmental elements like barometric pressure changes are often reported to worsen symptoms, although scientific evidence varies.
How Arthritis Is Diagnosed
Accurate arthritis diagnosis begins with a physical examination assessing swelling and range of motion. Providers evaluate pain patterns and identify whether symptoms suggest a mechanical or inflammatory origin.
Imaging tests such as X-ray, Ultrasound, Magnetic resonance imaging (MRI), and Computed tomography (CT) scan reveal structural changes. Blood tests detect inflammatory markers, autoimmune indicators, or elevated uric acid levels.
Clear differentiation between degenerative and inflammatory forms ensures appropriate treatment selection.
Treatment and Management Options
Effective arthritis treatment aims to reduce pain, preserve function, and slow structural damage.
Medications for Arthritis
First-line therapies include NSAIDs, Acetaminophen, and prescription anti-inflammatory medicine. In inflammatory types, Corticosteroids and Cortisone shots reduce acute swelling. Long-term control of autoimmune inflammation may require DMARDs.
Medication plans are individualized based on severity and response.
You may also like: Masgonzola
Surgery and Advanced Treatments
When conservative approaches fail, surgery may be necessary. Joint fusion stabilizes damaged joints, particularly in the ankle or spine, including Spinal fusion or Ankle fusion.
Severe structural damage may require Arthroplasty, commonly known as Joint replacement, where a damaged joint is replaced with a prosthetic joint or artificial joint. Recovery and joint replacement recovery outcomes have improved significantly with modern surgical techniques.
Lifestyle Changes and Prevention Strategies
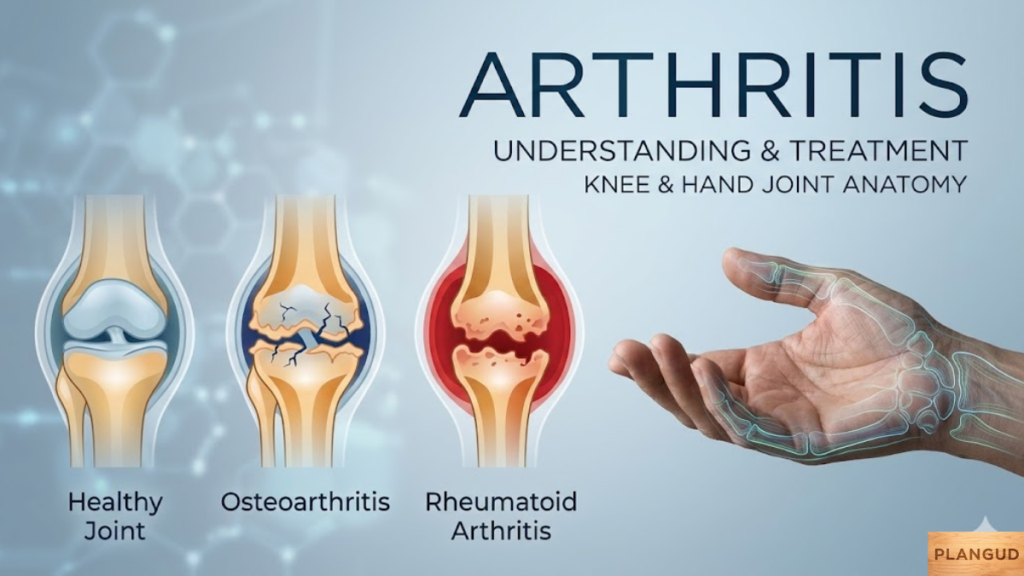
Proactive lifestyle management supports long-term arthritis prevention and symptom control. Regular low-impact exercise such as walking, swimming, or cycling strengthens surrounding muscles and enhances joint mobility.
Structured physical therapy and occupational therapy improve strength and coordination while protecting joint structures. Maintaining a healthy weight reduces joint stress, and avoiding tobacco lowers systemic inflammation.
Many individuals who remain active report fewer severe flare-ups and improved long-term mobility compared to sedentary patients.
Conclusion
Arthritis is a multifaceted chronic joint condition that can range from mild stiffness to advanced joint damage requiring arthroplasty or joint replacement. Whether driven by cartilage wear and tear, autoimmune disease, or hyperuricemia, early recognition and structured management significantly improve long-term outcomes.
Understanding arthritis symptoms, pursuing a timely arthritis diagnosis, and following personalized arthritis treatment strategies reduce progression and maintain independence. With informed medical guidance and consistent lifestyle support, most individuals successfully manage symptoms and preserve quality of life.
FAQs
1. What is the main cause of arthritis?
The main cause of arthritis depends on the type. Osteoarthritis develops from long-term cartilage wear and aging, while Rheumatoid arthritis is caused by immune system dysfunction. Other forms, such as Gout, result from high uric acid levels in the blood.
2. Can arthritis go away on its own?
No, arthritis is typically a chronic condition and does not go away permanently. However, symptoms can be managed effectively with medication, physical therapy, and lifestyle changes. Early treatment significantly slows progression and reduces joint damage.
3. How do I know if my joint pain is arthritis or something else?
Arthritis pain usually includes stiffness, swelling, and reduced range of motion that lasts for weeks or longer. If joint pain persists, worsens in the morning, or limits daily activities, a medical evaluation with imaging or blood tests is recommended. Only a proper diagnosis can confirm the exact cause.
4. At what age does arthritis usually start?
Arthritis can begin at any age, but Osteoarthritis is most common after age 50. Rheumatoid arthritis often develops between ages 30 and 60, while Juvenile arthritis affects children under 16. Age of onset varies depending on the type and risk factors.
5. When should I consider joint replacement surgery?
Joint replacement is usually considered when severe pain and stiffness continue despite medication, therapy, and lifestyle changes. If arthritis significantly limits mobility or daily function, an orthopedic specialist may recommend arthroplasty. Surgery is typically the last option after conservative treatments fail.
Share this content: